|
8/22/2023 0 Comments Hippus pupil reaction 
Pupillary hippus (PH) refers to spontaneous bilateral synchronous rhythmic constriction and dilatation of the pupils. If the right side of the neck is subjected to a painful stimulus, the right pupil dilates (increases in size 1-2mm from baseline). The ciliospinal reflex (pupillary-skin reflex) consists of dilation of the ipsilateral pupil in response to pain applied to the neck, face, and upper trunk. What causes pupillary hippus? What happens in the Ciliospinal reflex? It has been hypothesized that it reflects a dysregulation of central parasympathetic nervous system activity. Pupillary athetosis-or hippus-is bilateral, rhythmic oscillations of the pupil regardless of light intensity. What causes abnormal pupillary reflex?Ībnormal pupillary light reflex can be found in optic nerve injury, oculomotor nerve damage, brain stem lesions, such as tumors, and medications like barbiturates. Sometimes your pupils can dilate without any change in the light. When it’s bright, they get smaller, or constrict, to let in less light. In low light, your pupils open up, or dilate, to let in more light. Partial anhidrosis involving only the medial aspect of the forehead ipsilateral side of the nose is associated with a lesion distal to the carotid bulb.Your pupils get bigger or smaller, depending on the amount of light around you. Anhidrosis of the entire face is often associated with a lesion at the level of the carotid artery. The pattern of anihidrosis may help identify the lesion. Anhidrosis (decreased sweating): Also caused by a loss of sympathetic activity.This degree of miosis may be subtle and require a dark room. Miosis (pupillary constriction): A loss of sympathetic input causes unopposed parasympathetic stimulation which leads to pupillary constriction.Ptosis (drooping eyelid): The superior tarsal muscle requires sympathetic innervation to keep the eyelid retracted.Loss of sympathetic innervation causing the clinical triad of: When light reaches a pupil there should be a normal direct and consensual response.Īn RAPD is diagnosed by observing paradoxical dilatation when light is directly shone in the affected pupil after being shown in the healthy pupild to be from a pathologic process Swing a light back and forth in front of the two pupils and compare the reaction to stimulation in both eyes. The swinging flashlight test is helpful in separating these two etiologies as only patients with optic nerve damage will have a positive RAPD. However, it will constrict if light is shone in the other eye (consensual response). If an optic nerve lesion is present the affected pupil will not constrict to light when light is shone in the that pupil during the swinging flashlight test. 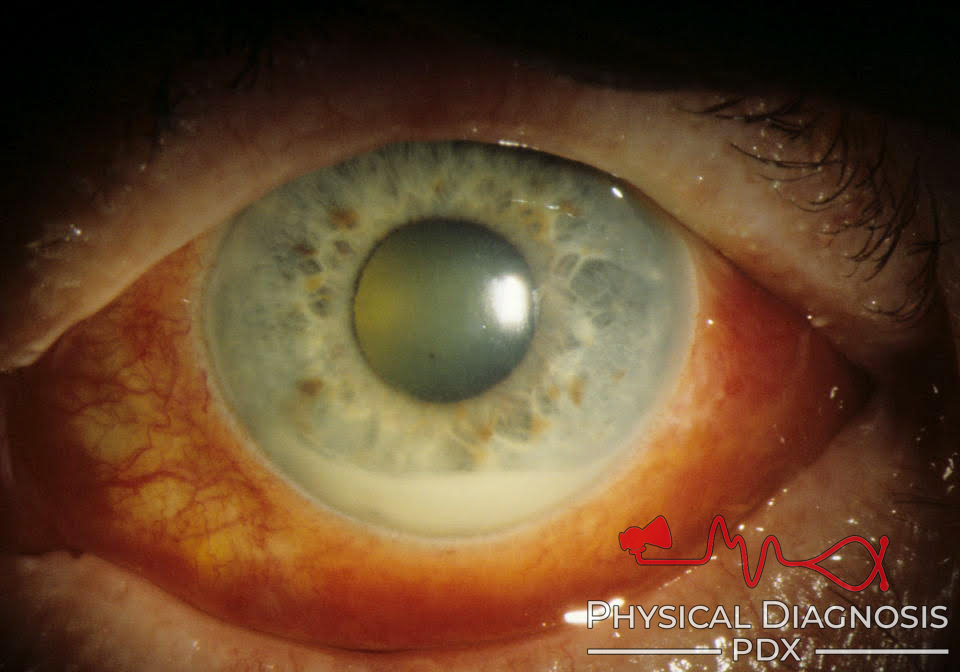
It is important to be able to differentiate whether a patient is complaining of decreased vision from an ocular problem such as cataract or from a defect of the optic nerve. It is due to damage inoptic nerve or severe retinal disease. Relative Afferent Pupillary Defect (RAPD, Marcus Gunn Pupil)Īn RAPD is a defect in the direct response. 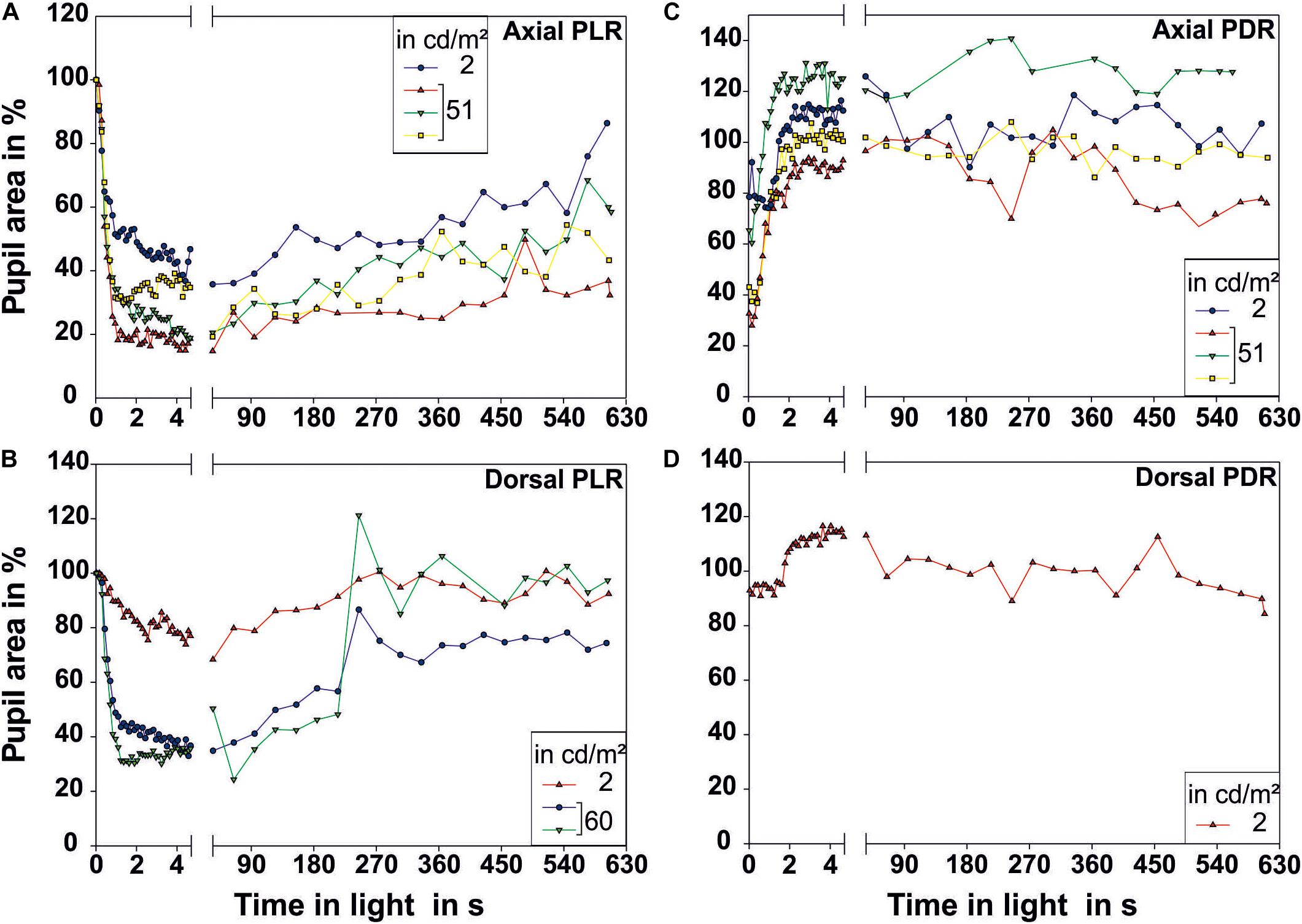
They synapse at the superior cervical ganglion where third-order neurons travel through the carotid plexus and enter into the orbit through the first division of the trigeminal nerve. Post synaptic neurons travel down all the way through the brain stem and finally exit through the cervical sympathetic chain and the superior cervical ganglion. Sympathetic innervation begins at the cortex with the first synapse at the cilliospinal center (also known as Budge's center after German physiologist Julius Ludwig Budge). Dilation is controlled by the dilator pupillae, a group of muscles in the peripheral 2/3 of the iris. Sympathetic innervation leads to pupillary dilation. 
The fibers enter the orbit with CNIII nerve fibers and ultimately synapse at the cilliary ganglion. The pathway of pupillary constriction begins at the Edinger-Westphal nucleus near the occulomotor nerve nucleus. The fibers of the sphincter pupillae encompass the pupil. A circular muscle called the sphincter pupillae accomplishes this task. Parasympathetic innervation leads to pupillary constriction. The physiology behind a "normal" pupillary constriction is a balance between the sympathetic and parasympathetic nervous systems. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
